 Insufficient dietary vitamin D intake (below the estimated average requirement of 10 μg/day) exists within populations around the globe, further exacerbating the vitamin D deficiency pandemic. The global prevalence of vitamin D deficiency and insufficiency (defined as serum 25 hydroxyvitamin D < 30 and 30–50 nmol/L) ranges from ~5–18% to 24–49%, respectively, depending on the study region and population. The proposed combination of typically altered mineralization markers for the diagnosis of osteomalacia is, at best, suggestive until further comparisons with established diagnostic tools (histological analysis of bone biopsies) are conducted. Screening of apparently healthy Arab adolescents revealed a high prevalence of deranged mineralization markers suggestive of biochemical osteomalacia, which was significantly more common in girls than boys and was likely associated with Arab traditional clothing and diet. Overall, girls were 4.6 times (95% CI 3.3–6.4) more likely to have biochemical osteomalacia than boys. The prevalence of low serum Ca and/or Pi was also higher in girls than in boys (24.2% vs. The overall prevalence of biochemical osteomalacia was 10.0% (n = 295/2938) and was higher in girls than boys (14.7% vs. Vitamin D deficiency was noted in 56.2% (n = 953) of girls and 27.1% (n = 336) of boys ( p < 0.001). A total of 2938 Arab adolescents were recruited. Biochemical osteomalacia was defined as any two of the following four serum markers of hypomineralization, namely low 25 hydroxyvitamin D (25OHD < 30 nmol/L), high alkaline phosphatase (ALP), low calcium (Ca), and/or inorganic phosphorous (Pi). Anthropometrics and fasting blood samples were collected. In this cross-sectional study performed between September 2019 and March 2021, adolescents aged 12–17 years from 60 different secondary and preparatory year schools in Riyadh, Saudi Arabia were included. This study assessed the prevalence of biochemical osteomalacia in Arab adolescents. Establishing less invasive, cheap, and widely available diagnostic markers for this underdiagnosed entity is essential, in particular for screening in high-risk groups. Moreover, fortification of foodstuff with vitamin D is lacking in India.Nutrition-acquired osteomalacia is a bone mineralization disorder associated with dietary calcium and/or solar vitamin D deficiency, risk factors considered common in the Middle Eastern region. Reduced outdoor exposure to sunlight due to the prevailing COVID-19 pandemic perhaps resulted in severe vitamin D deficiency. 4 The finding is more commonly seen in younger children and is unusual at the age of our patient. 1 It gives rise to frayed appearance of the metaphyses on radiographs. 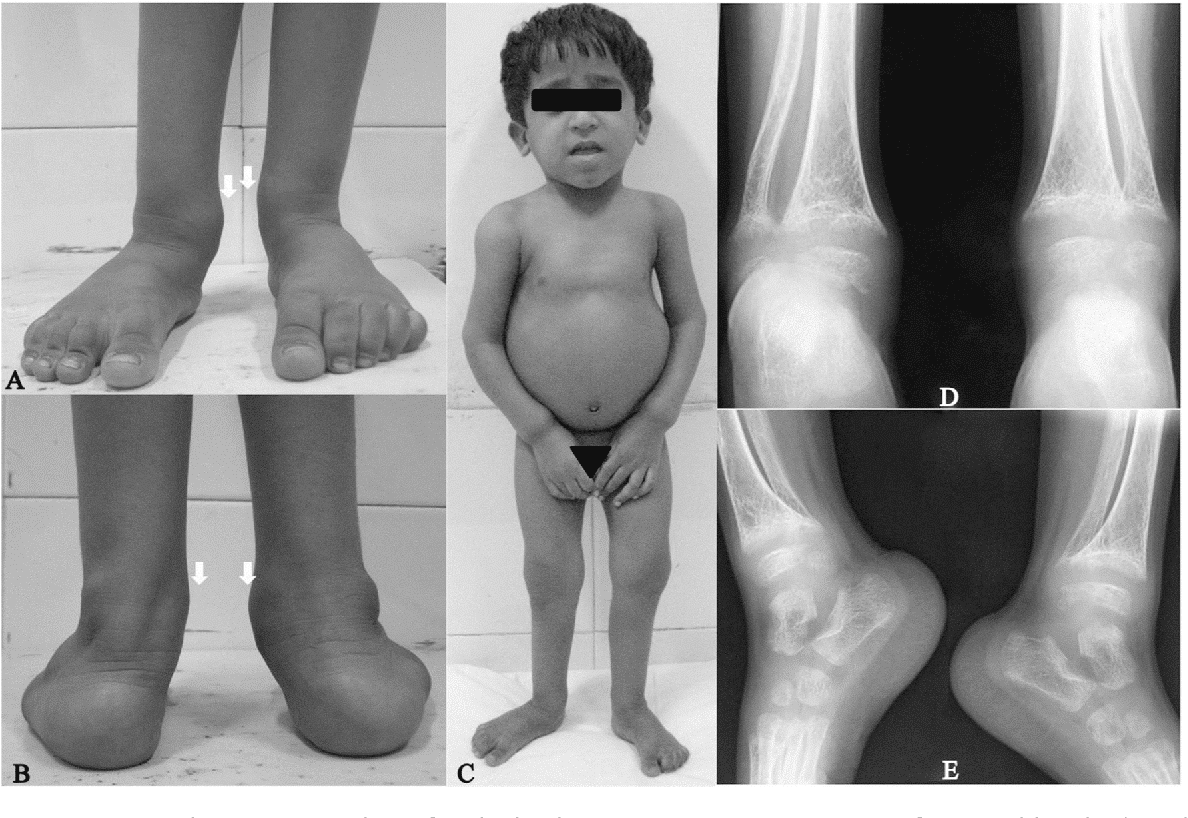
3 Abnormal ossification of the growth plate in growing children is the hallmark of the disease. However, older children present more often with proximal muscle weakness, fatigue, and pain in the joints and muscles. Bowing of legs, widening of wrists, rachitic rosaries, and Harrison sulcus are some of the well-known deformities. 2 Various skeletal deformities are seen due to suboptimal bone strength. Rickets is more common in younger children (mean age 1.4 years in a study from New Zealand). 
1 Mutations of the genes involved in the metabolism of calcium, vitamin D, and phosphorus are rare causes. Vitamin D deficiency is a common cause of nutritional rickets in tropical countries. It occurs due to the deficiency of calcium and/or phosphate, required for mineralization of the bones. Rickets is a metabolic bone disease seen in children. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
